If you’re tired of hearing that weight loss is just about discipline or that failing to shed pounds is a moral failing, you’re not alone. The relentless emphasis on willpower often overlooks the complex biological, psychological, and societal factors at play. This comprehensive guide challenges common misconceptions around obesity, explores the science behind weight management, and offers actionable insights to support a more compassionate approach.
The Hidden Layers of Obesity: Disease, Trauma, and Inflammation
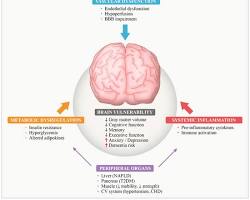
Obesity isn’t simply a matter of eating too much or moving too little. It is a chronic relapsing disease characterized by ongoing biological processes that resist quick fixes. The Disease Model of Obesity. Many medical organizations recognize obesity as a disease—an active, inflammatory endocrine disorder. Excess adipose tissue secretes cytokines, which promote inflammation and disrupt normal hormonal signals like leptin and insulin. These disruptions lead to increased hunger, decreased satiety, and metabolic resistance, making weight loss more complicated than calories in versus calories out. Trauma and Obesity Connection Anecdotal evidence suggests a significant link between trauma—such as sexual harassment or childhood abuse—and obesity, especially in women. Trauma can lead to emotional eating or weight gain as a protective mechanism against psychological distress. Addressing trauma is crucial for long-term weight management, yet it remains overlooked in traditional weight loss paradigms.
Rethinking Weight Loss: Willpower vs. Biological Reality
The prevailing view that weight loss is purely about discipline ignores the biology that works against us. Remember, obesity involves complex feedback loops:
- Metabolic Adaptation: Every effort to lose weight triggers the body’s survival mechanisms, which reduce energy expenditure and increase hunger.
- Set Point Theory: Your body resists permanent weight change by adjusting internal signals, making long-term maintenance challenging.
- Inflammation: Excess fat contributes to systemic inflammation, further disrupting metabolism and hormones like insulin, leptin, and ghrelin.
This opposition explains why many people struggle despite their best efforts, and why punitive “eat less, move more” advice often backfires.
The Power of Medications and Lifestyle Medicine
Fortunately, advances in pharmacology are transforming obesity treatment. Drugs like GLP-1 receptor agonists (e.g., Wegovy, Ozempic, Tirzepatide) have shown remarkable effectiveness in suppressing appetite, reducing weight, and improving metabolic health. How Do GLP-1 Medications Work? Originally developed for diabetes, these medications impact gut-brain signaling pathways that regulate hunger and satiety. They not only facilitate weight loss but also confer cardioprotective benefits, especially in postmenopausal women. The Question of “Cheating” Using medication to manage hunger is not cheating—it’s utilizing available tools to improve health, much like someone with diabetes uses insulin. Obesity is a disease; treating it with medications should be normalized, not stigmatized.
The Psychological Dimension: Self-Love and Support
Addressing weight from a purely physical perspective neglects the critical psychological elements. Self-compassion, positive body image, and supportive communities are foundational for sustainable change. Love Yourself at Every Size. Stepping into a healthier weight involves not only physical adjustments but also reshaping internal narratives. Recognize your worth regardless of size, and practice self-love as you pursue health. Cultivating Support Systems: Surround yourself with people who uplift you—support groups, friends, or healthcare providers who understand the science and prioritise your well-being. Avoid environments that promote food noise or shame.
The Intersection of Society, Media, and Beauty Standards
Cultural standards heavily influence perceptions of beauty, often to the detriment of health. The glorification of thinness, unrealistic ideals, and diet culture can lead to disordered eating, shame, and mental health struggles. Recognizing and challenging these narratives is part of the journey toward holistic health.
Moving Forward: Practical Steps for Sustainable Weight Management
- Get a Comprehensive Medical Evaluation
Understand your hormonal health, inflammation markers, and any underlying conditions. Collaborate with providers who acknowledge obesity as a disease. - Consider Medication as Part of Your Toolkit
Informed discussions with a knowledgeable healthcare provider can open doors to medications like GLP-1 agonists, which have been proven safe and effective for many. - Address Psychological and Trauma-Related Factors
Seek professional help if trauma or emotional eating impedes your progress. Supporting mental health is key to physical changes. - Adopt a Compassionate, Sustainable Lifestyle
Emphasize whole foods, manageable activity, hydration, sleep, and stress management. Extinguish food noise and nurture your self-esteem. - Build a Supportive Community
Engage with groups or professionals who reinforce positive change without shame or blame.
Final Thoughts: Embrace the Journey of Self-Care
The path to health is iterative, often non-linear, and uniquely yours. It requires embracing science, compassion, and patience. Remember—your worth isn’t defined by a number on the scale. If you’re considering medical intervention to support your weight loss journey, do so with informed guidance and self-love at the forefront. Treatment is about reclaiming your health, not conforming to societal pressures.
Watch the full conversation: here
Want to learn more about body positivity and health?

About Dr. Michelle Gordon
Dr. Michelle Gordon (affectionately known as “Dr. G”) is a board-certified former surgeon who traded the operating room for a mission to transform metabolic health. After spending 15 years running a multi-million dollar surgical practice, Dr. Gordon experienced a profound life “relaunch” following burnout and the COVID-19 pandemic. Today, she is a leading expert in Menopause Management, Medical Weight Loss, and Lifestyle Medicine.
As the founder of The Menopause Movement and The Meno System, she specializes in de-stigmatizing obesity by treating it as a complex biological disease rather than a character flaw. Her holistic “Kitchen Therapy” approach empowers women and high achievers to reclaim their health through mindset, habit change, and sustainable behavior modification.
Connect with Dr. Gordon:
- Official Website: drmichellegordon.com
- Coaching & Programs: drgordon.me
- Podcast: Launch Your Life with Dr. Michelle Gordon
- Instagram: @drmichellegordon
- LinkedIn: Dr. Michelle Gordon
- Facebook: @doctormichellegordon
Frequently Asked Questions
Is weight loss solely about willpower?
Not at all. Obesity involves complex hormonal, inflammatory, and psychological factors. Willpower alone cannot overcome biological resistance—medications and supportive lifestyle changes are essential.
Can trauma really influence weight?
Yes. Trauma, especially in women, has been linked to emotional eating, weight gain, and altered cortisol levels, which promote visceral fat accumulation.
Are medications like GLP-1 safe long-term?
Research indicates that GLP-1 receptor agonists are safe for long-term use under medical supervision, with additional benefits like improved cardiovascular health.
Does menopause make weight loss harder?
Absolutely. Hormonal fluctuations during menopause and perimenopause promote visceral fat accumulation and metabolic shifts that challenge weight management efforts.
Is it too late to start hormone therapy or medications?
Not at all. Early or late, individualized treatment plans can improve quality of life, reduce health risks, and support sustainable weight management.
Remember:
Your health journey is unique and sacred. Seek support, prioritize self-love, and use all available tools to thrive.